If you’re worried about your drinking habits, watch for these early warning signs of alcohol addiction: bloodshot eyes, declining personal hygiene, unexplained weight changes, and withdrawal from activities you once enjoyed. You might notice you’re hiding alcohol consumption, experiencing tremors between drinks, or needing more to achieve the same effects. Mood swings, personality changes, and continuing to drink despite consequences are also red flags. Understanding each warning sign can help you determine when it’s time to seek professional help.
Bloodshot Eyes and Changes in Physical Appearance
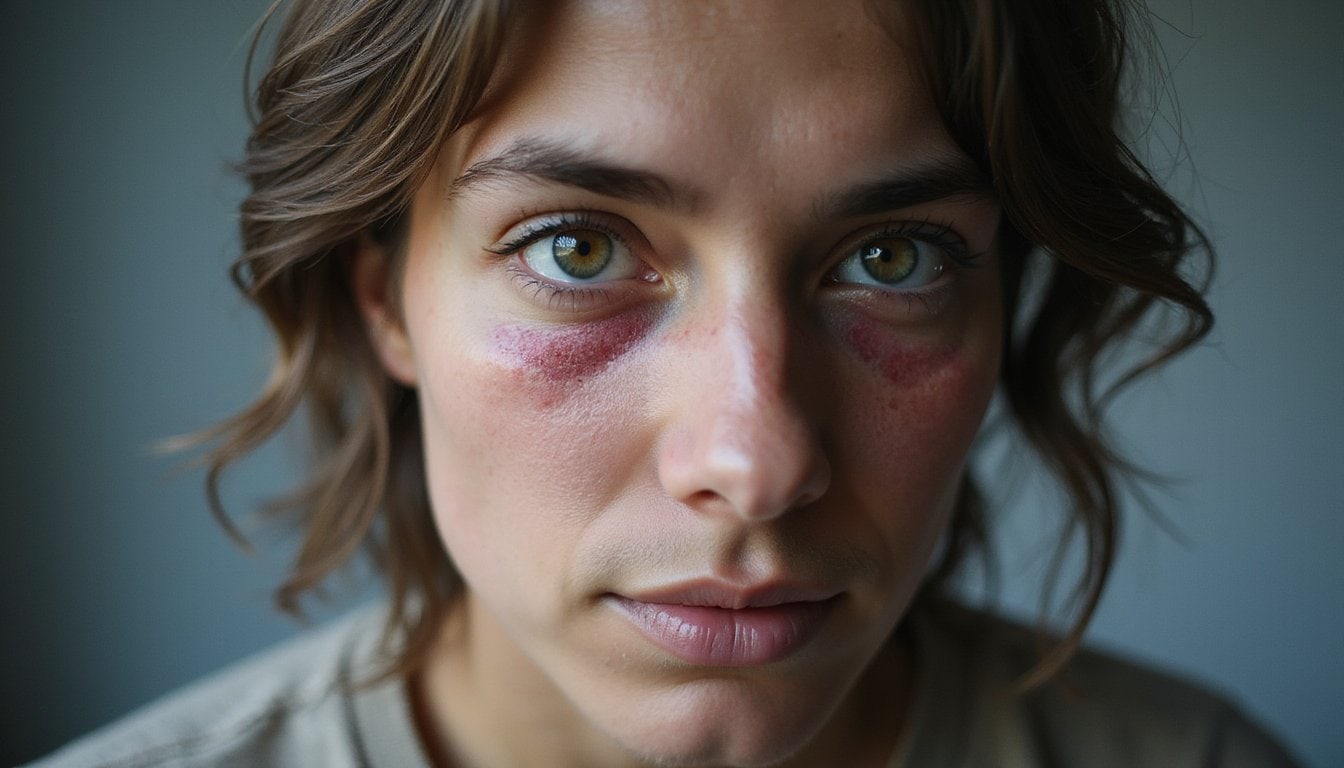
Bloodshot eyes often serve as one of the earliest visible indicators of problematic alcohol use. When you drink heavily, blood vessels in your eyes dilate, causing redness and a swollen appearance. While casual drinkers experience temporary symptoms that resolve within 24 hours, persistent bloodshot eyes signal frequent heavy drinking or developing addiction.
You’ll also notice significant pupil and iris changes. Heavy alcohol consumption slows your iris’s ability to constrict and dilate properly, leading to light sensitivity issues and poor night vision. Your contrast sensitivity can decrease by up to 30%, making nighttime driving dangerous. Additionally, heavy drinking causes reduced corneal sensitivity, which can mask pain from potential eye injuries or infections.
Long-term physical changes include puffy, red eyes with spider-like blood vessels and small hemorrhages on the eye surface. Prolonged alcohol use has also been linked to serious conditions such as age-related macular degeneration, cataracts, and even alcohol blindness. These visible markers indicate internal health deterioration that shouldn’t be ignored.
Neglecting Personal Grooming and Hygiene Habits
When you notice someone skipping showers, wearing the same unwashed clothes repeatedly, or abandoning basic grooming routines they once maintained, these behavioral shifts often signal alcohol addiction’s grip on daily functioning. Research indicates that individuals with hazardous drinking patterns show markedly elevated odds of neglectful behaviors (OR 2.89, 95% CI 1.74-4.80), with prioritization of alcohol consumption displacing self-care activities. You’ll observe visible indicators like disheveled hair, body odor, and unkempt clothing as the addiction progressively erodes motivation for hygiene maintenance. Studies show that daily alcohol consumption independently increases the odds of neglectful behaviors on the same day, creating a cycle where drinking directly interferes with routine self-care. The physical toll extends beyond hygiene habits, as chronic alcohol abuse leads to dry, flaky skin and premature wrinkles that become increasingly noticeable over time.
Declining Daily Hygiene Routines
How does alcohol addiction quietly erode the most basic self-care habits you’ve maintained for years? When substance dependence takes hold, your brain deprioritizes hygiene as judgment and motivation decline. You’ll notice bathing becomes irregular, leading to bacterial growth, skin infections, and potential abscesses, particularly if you’re injecting substances.
Your brushing patterns shift diagnostically. Research shows alcohol-dependent individuals brush with hard toothbrushes at statistically significant rates (p=0.039), yet this produces no measurable oral health improvement. You might brush frequently, 59% report brushing more than once daily, but impaired motor activity renders the effort ineffective. Studies reveal that none reported flossing, indicating a complete absence of interproximal cleaning among this population.
The consequences compound. Neglected hygiene contributes to chronic pain, systemic health deterioration, and threefold higher rates of permanent tooth loss. Financial instability redirects resources from soap and toothpaste toward alcohol, accelerating this decline in self-care routines. As appearance deteriorates, many individuals avoid social gatherings due to embarrassment, deepening the cycle of isolation and shame.
Unkempt Physical Appearance
As alcohol dependence progresses beyond declining hygiene routines, your physical appearance broadcasts visible warning signs that others often notice before you do. Altered self grooming practices manifest through disheveled hair, unkempt clothing, and an exhausted appearance. Nutrient deficiencies cause brittle, thinning hair, while chronic dehydration accelerates premature graying.
| Physical Indicator | Primary Cause | Clinical Significance |
|---|---|---|
| Disheveled hair | Protein/zinc deficiency | Nutritional compromise |
| Body odor | Alcohol metabolites in sweat | Metabolic dysfunction |
| Unkempt clothing | Priority displacement | Behavioral deterioration |
Deteriorating personal hygiene becomes evident through persistent body odor from alcohol excretion through skin and infrequent bathing. Your gaunt facial features and puffy eyes reflect malnutrition and sleep disruption. Stained, wrinkled clothing signals that addiction now supersedes basic self-care maintenance. Poor oral hygiene and tooth decay from acidic alcoholic beverages further contribute to the overall neglected appearance. Research indicates that individuals with histories of childhood physical neglect experience poorer mood and higher stress daily, which may compound self-care deterioration when combined with alcohol dependence.
Ignoring Self-Care Basics
Nearly two-thirds of individuals with alcohol use disorder report that physical health impacts directly interfere with their ability to maintain daily hygiene routines. When you’re struggling with dependence, basic grooming becomes secondary to obtaining and consuming alcohol. Research shows 16.6% of those with physical dependence prioritize drinking over self-care activities.
Sustained hygiene lapses often indicate deepening addiction. You may notice showering, brushing teeth, or changing clothes becomes irregular or abandoned entirely. Self medication hygiene impacts compound these deficits, those using alcohol to manage mood symptoms face triple the odds of developing dependence, perpetuating neglect cycles. Physical deterioration extends beyond grooming, as chronic alcohol use can weaken the immune system, making individuals more susceptible to illness and further compromising their ability to maintain self-care routines.
With only 7.2% of affected individuals receiving treatment, these patterns frequently persist unchecked. Problem severity directly predicts impairment in daily functioning, making hygiene deterioration a reliable diagnostic marker for escalating alcohol use disorder. However, approximately 70% of persons with AUD and alcohol problems improve without formal interventions through natural recovery, suggesting that early recognition of warning signs like hygiene neglect can prompt self-correction before treatment becomes necessary.
Sudden Unexplained Weight Loss or Gain
Unexpected shifts in body weight often signal problematic alcohol consumption patterns. You’ll notice that heavy drinkers achieve only 2.4% weight loss compared to abstainers’ 5.1% over four years. Alcohol triggers uncontrollable appetite fluctuations, end-of-treatment alcohol intake correlates positively with non-alcohol energy consumption. Irregular sleep patterns compound these metabolic disruptions.
Key diagnostic indicators include:
- Caloric surplus: Consistent-light drinkers consume 182.8 extra kcals daily versus abstainers
- Impaired weight management: Only 4.8% of heavy drinkers achieve ≥10% weight loss compared to 27.5% of abstainers
- Disinhibited eating: Higher impulsivity levels amplify overeating risk when alcohol’s present
You’re facing increased difficulty maintaining healthy weight because alcohol adds direct calories while simultaneously lowering dietary restraint. Research conducted at the University of Pennsylvania examined how alcohol intake affects weight loss outcomes during intensive lifestyle interventions for adults with overweight. The encouraging news is that participants who consumed alcohol at baseline meaningfully reduced their intake by the end of behavioral weight loss treatment. These metabolic warning signs warrant immediate clinical evaluation for developing alcohol dependence.
Withdrawing From Hobbies and Social Activities

Withdrawing from hobbies and social activities represents one of the most observable behavioral markers of developing alcohol dependence. You may notice that activities you once enjoyed no longer hold appeal as drinking becomes your primary focus. Time previously dedicated to recreation redirects toward alcohol acquisition and consumption, leading to compromised productivity across multiple life domains.
Research demonstrates that socially isolated individuals exhibit alcohol use disorder rates of 14.4% compared to 4.9% in non-isolated populations. As you withdraw from established social networks, strained family relationships often follow. This isolation creates a bidirectional cycle, loneliness increases high-risk drinking patterns, while continued alcohol use pushes away remaining support systems. Studies show that lonely individuals who were previously non-high-risk drinkers were 45% more likely to progress to high-risk drinking patterns over a one-year period. The abandonment of leisure pursuits and social connections removes protective factors that typically moderate drinking behavior. However, some research indicates that loneliness is associated with less frequent drinking rather than increased consumption, suggesting the relationship between social isolation and alcohol use is complex.
Drinking Alone and Hiding Alcohol Consumption
How frequently you consume alcohol in solitude, and whether you’ve begun concealing this behavior, serves as a critical diagnostic indicator for developing alcohol use disorder. Research shows 25% of individuals actively hide their intake from others, with 10 million Americans qualifying as hidden alcoholics.
Hiding how much you drink? You’re not alone, 25% of people conceal their alcohol consumption from others.
Key warning signs include:
- Hiding alcohol in plain sight within containers like travel mugs, water bottles, or refilled liquor bottles
- Disappearing frequently to bathrooms, vehicles, or bedrooms for secretive consumption
- Lying about quantities consumed or whereabouts when drinking
- Stashing bottles in unexpected locations such as toilet tanks, behind books, inside furniture, or within spare tire compartments
Covering up alcohol consumption often stems from shame, guilt, and denial, psychological drivers that perpetuate the addiction cycle. You may rationalize this behavior as emotional coping, but secretive drinking patterns signal dependency requiring clinical evaluation. If you’re discovering empty containers in unusual locations, seek professional assessment immediately.
Inability to Control How Much or How Often You Drink

When you consistently drink more than you intended, or find yourself unable to stop once you’ve started, you’re experiencing a hallmark symptom of alcohol use disorder. This loss of control affects 28.1 million U.S. adults, manifesting as drinking that overrides your planned limits despite negative consequences.
Your preoccupation with obtaining alcohol often leads to missed social commitments and strained relationships. You may notice tolerance developing, needing more alcohol to achieve previous effects. Research shows 10% of binge drinkers develop dependence, with rates climbing to 30% among those who binge ten or more times monthly.
Negative emotions like stress emerge during abstinence, driving compulsive consumption cycles. If you cannot predict how much you’ll drink or when you’ll stop, this diagnostic marker warrants immediate clinical evaluation.
Experiencing Tremors and Physical Withdrawal Symptoms
When you notice your hands shaking 6-8 hours after your last drink, you’re experiencing one of the most telling physical indicators of alcohol dependence. These tremors typically accompany other withdrawal symptoms like sweating, nausea, and rapid heartbeat, signs that your body has become physiologically dependent on alcohol. Understanding when these symptoms escalate from uncomfortable to dangerous, particularly the progression toward delirium tremens in 5% of heavy drinkers, can be critical for your safety.
Recognizing Early Tremor Signs
Few physical symptoms signal alcohol dependence as clearly as tremors, the involuntary shaking that typically emerges 6-12 hours after your last drink. Recognizing early tremor patterns helps distinguish withdrawal from other conditions like hypoglycemia or anxiety disorders.
Key diagnostic indicators include:
- Small, rapid shaking concentrated in hands and fingers
- Worsening symptoms during fine motor tasks or reaching movements
- Accompanying signs such as sweating, elevated heart rate, and nausea
Peak severity occurs within 24-48 hours, with symptoms gradually subsiding over several days. You’ll notice that alcohol temporarily suppresses these tremors, a hallmark sign of physical dependence.
Early tremor management requires medical evaluation. These symptoms indicate CNS hyperactivity from disrupted neurotransmitter balance and may precede severe complications, including delirium tremens. Don’t attempt unsupervised detoxification.
Common Physical Withdrawal Symptoms
Physical withdrawal symptoms tend to set in 6-12 hours after your last drink, with tremors, sweating, and nausea marking the body’s initial response to alcohol absence. You’ll likely experience hand tremors, anxiety, insomnia, and poor appetite during this initial phase. Headaches and heart palpitations commonly accompany these early signs.
As withdrawal progresses between 12-48 hours, you’ll notice intensifying symptoms including increased blood pressure, rapid heart rate, and clammy skin. Heavy users show 95% higher likelihood of rapid heart rate and 69% increased sweating. Muscle spasms and breathing abnormalities emerge as your body struggles to recalibrate.
Symptoms peak at 24-72 hours, potentially including fever, confusion, and seizures. Physical symptoms typically resolve within 4.83 days on average, though 95% of cases clear between 2-8 days.
When Symptoms Become Dangerous
Most people experiencing alcohol withdrawal will navigate mild to moderate symptoms without life-threatening complications, but certain warning signs indicate you’ve crossed into dangerous territory.
You should seek immediate medical attention if you experience:
- Severe tremors persisting beyond 48 hours accompanied by worsening physical coordination
- Visual or auditory hallucinations signaling neurological escalation
- Fever with irregular heart rate indicating delirium tremens onset
Delirium tremens emerges 2-3 days after cessation, progressing from insomnia and seizures to clouded consciousness and disorientation. This condition carries heightened health risks and proves potentially fatal without intervention.
Your body’s neurological imbalance, excess glutamate combined with reduced GABA, creates dangerous overexcitation. Seizures or loss of consciousness demand emergency care. Don’t dismiss worsening symptoms as typical withdrawal; they require clinical evaluation.
Needing More Alcohol to Feel the Same Effects
When your body requires increasing amounts of alcohol to achieve the same buzz or relaxation you once felt with smaller quantities, you’re experiencing tolerance, a key neurobiological adaptation that signals your brain has begun rewiring itself in response to repeated alcohol exposure.
This increasing dose pattern emerges through two primary pathways: functional tolerance, where you behaviorally adapt despite elevated blood alcohol levels, and metabolic adaptations involving liver enzyme induction that accelerates alcohol breakdown. Your alcohol dehydrogenase activity intensifies with repeated exposure, processing alcohol faster than before.
Clinical indicators include consuming past 0.05 BAC without typical impairment, shifting from casual sips to heavy episodes in compressed timeframes, and drinking larger quantities without apparent drunkenness. Research shows 74.63% of individuals progress to heavy drinking once this escalation begins. Rising tolerance directly predicts alcohol use disorder development.
Dramatic Mood Swings and Personality Changes
Beyond the physical tolerance markers, alcohol’s neurological impact often manifests through observable shifts in temperament and behavioral patterns that you or those around you may notice. Research demonstrates that chronic alcohol use produces measurable changes in temperament, including heightened neuroticism and reduced emotional stability.
Watch for these diagnostic indicators:
- Increased anxiety and paranoia, you may experience elevated baseline nervousness between drinking episodes
- Erratic mood variations, sudden shifts from mild-mannered behavior to aggression or hostility emerge
- Decreased conscientiousness, you struggle with impulse control and follow-through on commitments
These personality alterations aren’t character flaws, they’re neurological consequences. Studies show alcohol dependence accelerates neuroticism increases while diminishing extraversion and sociability. You might notice heightened sensation-seeking behaviors and reduced emotional regulation. These erratic mood variations signal your brain chemistry is adapting to alcohol’s presence.
Continuing to Drink Despite Negative Consequences
When you continue drinking despite clear health consequences, knowing alcohol contributes to 2.6 million annual deaths worldwide, you’re exhibiting a core diagnostic criterion for alcohol use disorder. You may find yourself risking relationships anyway, even as loved ones express concern about behavioral changes or the 696,000 annual assaults linked to peer drinking. Prioritizing alcohol over responsibilities signals that dependence has begun overriding your decision-making capacity, regardless of mounting personal and social costs.
Ignoring Health Consequences
Despite clear medical evidence linking alcohol to serious organ damage, many individuals continue drinking even after receiving diagnoses that should prompt immediate cessation. You might dismiss lasting health impacts as distant concerns, yet 50.3% of cirrhosis deaths in 2023 were alcohol-related. This denial pattern signals addiction progression.
Key diagnostic indicators include:
- Continued consumption after liver disease diagnosis, despite 20-40% mortality rates within three months for severe alcohol-associated hepatitis
- Ignoring cardiovascular warnings while experiencing elevated blood pressure and cholesterol
- Dismissing cancer risk information, even knowing alcohol causes over 20,000 annual U.S. cancer deaths
Your health deterioration often coincides with financial instability from mounting medical costs. When you prioritize drinking over physician recommendations, you’ve crossed from casual use into addiction territory requiring immediate intervention.
Risking Relationships Anyway
The damage alcohol addiction inflicts on relationships often serves as one of the clearest diagnostic markers of disease progression. When you continue drinking despite damaged relationships, you’re exhibiting a hallmark symptom of alcohol use disorder. Research indicates verbal aggression doubles and physical aggression quadruples when alcohol enters conflict situations.
You’ll notice eroded emotional intimacy as drinking takes priority over commitments, anniversaries, and quality time with loved ones. Trust deteriorates through dishonesty about your whereabouts and companions. Partners often develop codependency, neglecting their own wellbeing while managing your addiction.
The statistics are stark: one-half of U.S. divorces involve alcohol misuse, and children in these households face twice the risk of developing substance use disorders themselves. If you’re sacrificing relationships for alcohol, this diagnostic criterion demands clinical attention.
Prioritizing Alcohol Over Responsibilities
Beyond damaged relationships, alcohol use disorder manifests through systematic neglect of life’s fundamental responsibilities, work, finances, family, legal obligations, and self-care. When you’re skipping work meetings, accumulating debt from alcohol purchases, or disregarding family needs, these behaviors signal diagnostic concern.
Clinical indicators include:
- Occupational dysfunction: Chronic absenteeism, missed deadlines, and impaired judgment causing workplace errors
- Financial deterioration: Prioritizing alcohol over essential bills, resulting in late fees and mounting debt
- Domestic neglect: Abandoning household duties, parental responsibilities, and family events
You may continue drinking despite DUI charges, court mandates, or medical warnings about liver disease, which accounts for 19.1% of alcohol-related deaths. This persistent disregard for consequences across multiple life domains represents a hallmark criterion for alcohol use disorder requiring professional assessment.
Frequently Asked Questions
How Long Does It Take for Alcohol Addiction to Develop?
You can develop alcohol addiction over several months to years, depending on your consumption patterns and personal risk factors. Frequent binge drinking accelerates this timeline dramatically. You’ll notice a gradual increase in tolerance, requiring more alcohol to achieve the same effects. Your progression isn’t uniform, genetic predisposition, mental health status, and drinking frequency all influence how quickly dependence forms. Early intervention during initial warning signs offers the best outcomes for preventing full addiction development.
Can Someone Be Genetically Predisposed to Alcohol Addiction?
Yes, you can be genetically predisposed to alcohol addiction. Research shows genetic factors account for 40-60% of your risk for developing alcohol use disorder. If you have a family history of alcoholism, your vulnerability increases substantially. Specific gene variants affecting alcohol metabolism, like ADH1B and ALDH2, directly influence your susceptibility. However, genetics aren’t destiny; they interact with environmental factors to determine your overall risk profile.
What Professional Treatment Options Are Available for Alcohol Addiction?
You have several evidence-based treatment options available. Inpatient rehabilitation programs provide 24/7 medically supervised care, ideal for severe AUD or withdrawal management. Intensive outpatient treatment offers structured therapy while you maintain daily responsibilities. FDA-approved medications can prevent relapse when combined with behavioral therapies like CBT or motivational enhancement. Your treatment team may include primary care providers, addiction specialists, or licensed therapists who’ll tailor interventions based on your diagnostic assessment and clinical needs.
How Can Family Members Help a Loved One With Alcohol Addiction?
You can provide emotional support by reinforcing positive sobriety-related behaviors while allowing natural consequences of drinking to occur. Encourage counseling through specific, positive requests for help-seeking rather than protective behaviors that shield from consequences. Research shows CRAFT (Community Reinforcement and Family Training) effectively teaches you communication skills and self-care strategies. Active partner coping predicts better drinking outcomes, and your positive support considerably improves recovery maintenance while enhancing overall family functioning.
Is It Dangerous to Quit Drinking Alcohol Cold Turkey?
Yes, quitting alcohol cold turkey can be extremely dangerous. You may experience severe withdrawal symptoms within 6-72 hours, including seizures, hallucinations, and delirium tremens, a potentially fatal condition. Your risk increases if you’ve been drinking heavily or have a history of withdrawal complications. You shouldn’t attempt detoxification without medical supervision, as healthcare providers can administer medications to prevent life-threatening complications and monitor your critical signs throughout recovery.

